Retinopathy of prematurity (ROP)
Retinopathy of Prematurity (ROP) is an eye problem that occurs in some babies and can lead to blindness.
 It is usually mild and often goes away on its own.
It is usually mild and often goes away on its own.
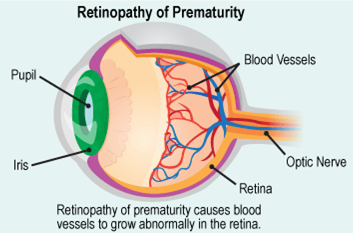
ROP affects the tissue inside the eye, at the back called the retina. The retina senses light and sends information to the brain for us to see.
In some premature babies, the blood vessels do not grow properly and develop the wrong way which can lead to scarring of the retina.
This is known as ROP.
Why do premature babies get ROP?
It is not fully understood why some babies get ROP.
Previously, ROP was linked with babies receiving oxygen and was more common. Now the amount of oxygen given to babies is carefully monitored and controlled. ROP is less common but still occurs.
If left unchecked, ROP can lead to blindness.
We know that the earlier and smaller babies are born, the higher the risk of developing ROP.
Risk factors include:
- how premature your baby is born
- the weight of your baby
- how unwell your baby has been.
Who gets screened?
If your baby was born before 31 weeks and/or weighing less than 1250g, they will be enrolled into the ROP screening program.
How often will my baby get screened?
The screening process happens every few weeks while your baby is in hospital. This is so we can check that your baby’s eye remains healthy at different stages of their eye growth.
If there is ROP, screening will happen more regularly, to make sure your baby’s vision stays safe.
How will I know if my baby has ROP?
There are no signs or symptoms when ROP develops. The only way to diagnose it is through eye examinations.
When will my baby have their eye test?
Our specialist nurses will arrange a week for the screening of your baby at 31 weeks or 4 weeks of age.
A special digital camera is used to take images of your baby’s retina. These images are reviewed by an eye specialist known as an Ophthalmologist, who will decide when further testing is needed.
Your baby will continue to have regular eye checks while they are in hospital, to make sure that their eyes are developing correctly.
What happens during the ROP test?
- About 1 hour before the examination, we will put drops in your baby’s eyes. The drops will make your baby’s pupils bigger. This allows photos of the retina to be taken so we can assess for ROP.
- The test will take place about 30 minutes before feeds and cares. Your baby can rest after the test. Older babies may be tested after a feed, so they are more settled. We will discuss the plan with you and your baby’s bedside nurse.
- Your baby will be swaddled to make them comfortable.
- We will give your baby sucrose to help with any discomfort they may feel.
- Next, we will put drops in your baby’s eyes that contain a local anaesthetic. This will make your baby’s eyes numb.
- Your baby’s eyelid will be held open with an eye lid speculum. This looks uncomfortable but it is important to remember that your baby’s eye is numb. The eyelids need to be out of the way so that good-quality photos can be taken.
- A water-based lubricating gel is applied to the top of your baby’s eye.
- The camera lens is used to look into the eye and take photos of the retina.
How long does the test take?
The test takes about 20 minutes from start to finish.
The eye lid speculum is used for less than 2 minutes in each eye.
Let your bedside nurse know if you would like to be present for your baby’s test.
Will my baby be in pain?
Your baby may cry when the light from the camera is put near their eye.
Swaddling, local anaesthetic eye drops, and sucrose are used to help keep your baby comfortable.
Your baby may be a bit light-sensitive for a few hours after the test.
When will my baby be seen?
The specialist ROP screening nurses will arrange for your baby’s eye test according to their birth gestation and weight.
This information sheet will be at your baby’s bedside on the Friday before your baby is examined.
If you have any questions, just ask the bedside nurse to contact the ROP screening team who are available Monday to Friday.
What happens after the ROP test?
All images taken by the ROP screening nurses will be assessed and reviewed by the Ophthalmologist.
Results will usually be available the following day.
The medical team or ROP screening nurses will talk to you about your baby’s results.
What happens if my baby has ROP?
Most cases of ROP heal without needing any treatment.
Your baby will be monitored more frequently as directed by the eye specialist.
In severe cases of ROP, the Ophthalmologist may suggest special medication injected into the eye or surgery. This will be discussed with you by your baby’s doctor and the Ophthalmologist.
What happens when my baby goes home?
Eye checks will continue after your baby goes home. All babies who have ROP screening will have at least one outpatient follow-up appointment at Perth Children’s Hospital (PCH).
In clinics, the Ophthalmologist does not use a camera to look into your baby’s eyes. They will use a special head light and open baby’s eyes with a gloved hand.
If your baby is returning to a regional area, an appointment may be made for your baby at Lion’s Outback Vision or by your local eye specialist. This is dependent on the availability and severity of ROP.
The team will let you know when your outpatient appointment will be before your baby goes home.
For metro area patients, you will receive a text message from PCH Ophthalmology clinic with the date and time of your baby’s appointment.
Attending clinic appointments after your baby is discharged is very important, even if your baby did not have ROP. Untreated ROP can lead to visual impairment or blindness.
DisclaimerThis publication is for general education and information purposes. Contact a qualified healthcare professional for medical advice. © State of Western Australia, Child and Adolescent Health Service Produced by: CAHS ROP Screening Team | Reference: 1986 | Last reviewed: 2026 |
This document can be made available in alternative formats on request.

